The body makes lots of sounds. Many of them are so quiet that we don’t normally hear them, and especially not in the middle of a noisy hospital. But even in the most routine medical visits, a physician can tell a lot about their patient by using a stethoscope to listen.
They can hear the heart beating, follow how well air is flowing in and out of the lungs, and monitor how food is moving along the gastrointestinal tract. And when things are blocked or not moving the way they should, that leaves audible clues, too.
An international team of researchers from McGill University, Northwestern University, and Hanyang University partnered to design and test noise-cancelling wearable devices to continuously monitor these sounds. Their study was published in Nature Medicine.
Existing digital stethoscopes are rigid, wired, and bulky. The team’s new acoustic device is designed to be worn on the skin to listen at strategic locations. Encased in soft silicone, each lightweight device is wireless and measures just 8 millimetres thick.
Packed into that small footprint are a flash memory drive, battery, accelerometer to measure movement, electronic components with bluetooth connectivity, and most importantly a pair of microphones with one facing toward the body and one facing out. The pair of microphones enables noise cancellation so that the internal body sounds can be heard.
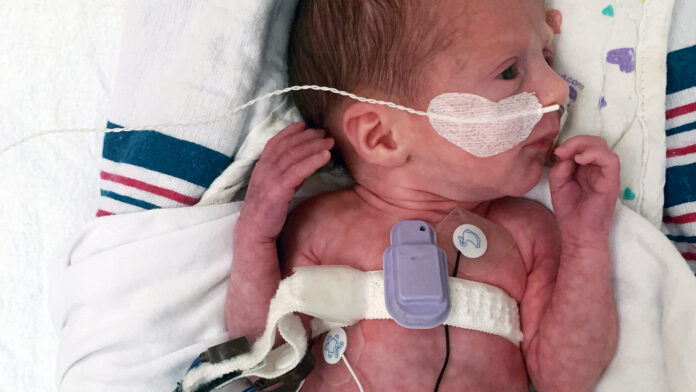
One application where this sensor is particularly useful is in monitoring premature babies in the neonatal intensive care unit (NICU). Premature babies often have trouble breathing, and apnea can occur when they stop breathing or something blocks their airflow.
Until now, there has been no way to continuously monitor airflow at the bedside in the NICU. In a pilot study of 15 infants, the team showed that when their acoustic device was worn on the chest just below the throat, it can not only monitor breathing, it can also accurately distinguish between apnea subtypes.
“The enhanced ability to detect and classify apneas could lead to more targeted and personalized care, improved outcomes and reduced length of hospitalization and costs,” said co-first author Wissam Shalish, assistant professor of pediatrics at McGill University and neonatologist at the Montreal Children’s Hospital, in a press release.
“When placed on the right and left chest of critically ill babies, the real-time feedback transmitted whenever the air entry is diminished on one side relative to the other could promptly alert clinicians of a possible pathology necessitating immediate intervention.”
The study also showed that the device could be used to monitor babies for intestinal blockages. In adults, who are larger and have more space to attach multiple devices, region-specific lung function could also be tracked after lung surgery.
Stethoscopes give physicians useful information on a broad variety of conditions, but they are often limited to being a snapshot in time. These sensors provide a non-invasive way to monitor the same sounds at multiple locations around the clock. For patients both big and small, this could be a new tool to help save lives.