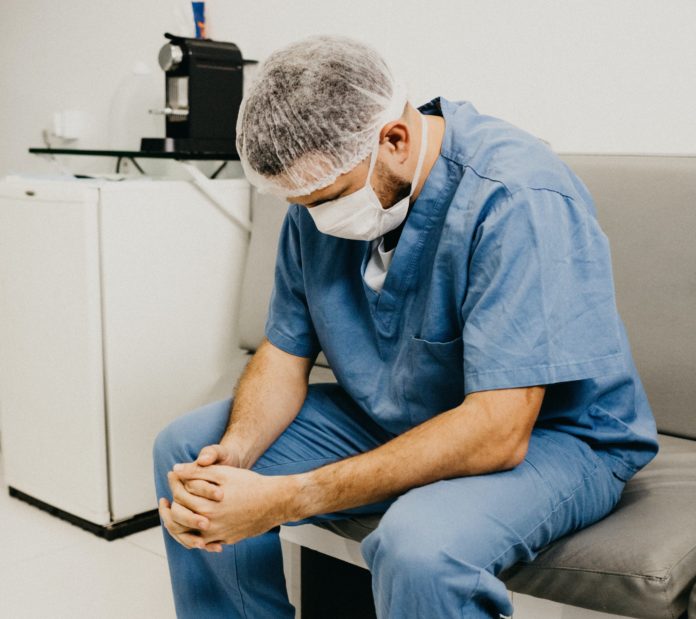
Many healthcare workers in the Toronto area today also worked on the front lines of the 2003 SARS outbreak — but does that past experience help them cope with the COVID-19 pandemic, or does it actually make them more likely to feel psychological distress?
These were the questions posed by a team of researchers from the University Health Network and the University of Toronto. By surveying nearly 4,000 healthcare workers from the Greater Toronto Area, the team was interested in learning whether employees present during SARS might face a higher risk of COVID-19 related emotional distress.
The study was led by Rima Styra, a Clinician Investigator at the Toronto General Hospital Research Institute, and published in PLOS ONE.
How does SARS experience affect workers’ mental health?
In 2003, the Greater Toronto Area was at the centre of a Severe Acute Respiratory Syndrome (SARS) outbreak. Like the COVID-19 pandemic, this presented significant mental health risks to frontline healthcare workers — and many employees present during the SARS outbreak are still employed in healthcare settings today.
Particularly prominent among these mental health risks was post-traumatic stress disorder (PTSD). This led the authors of the study to wonder whether dealing with the COVID-19 pandemic — another infectious disease outbreak — might trigger employees’ symptoms of mental distress.
“For [healthcare workers] who worked during the SARS outbreak, a recurrence or intensification of psychological distress may occur in response to exposure to a similar trauma, such as the COVID-19 pandemic,” the authors explained.
To determine whether or not this was the case, the researchers surveyed nearly 4,000 healthcare workers across the Greater Toronto Area, including nurses, non-clinical staff, allied health staff, and physicians. About 30 percent of the healthcare workers surveyed had worked during the 2003 SARS outbreak.
The team found that all healthcare workers surveyed — including those who had worked during SARS, and those who hadn’t — exhibited increased levels of mental distress.
More than half had moderate to severe scores for symptoms of PTSD, while a quarter showed increased levels of anxiety and more than 30% exhibited signs of depression.
While these findings are grim, the survey also revealed that healthcare workers who had gone through the SARS outbreak weren’t facing a greater toll on their mental health as a result.
“The results are both surprising and encouraging: previous work experience during the SARS outbreak did not result in increased psychological distress […] during the COVID-19 pandemic,” the authors said.
“These results are important as they can provide insights into how familiarity with outbreak management may temper negative mental health effects.”
Non-clinical healthcare workers face a particular risk
The authors went on to search for other factors that might have led to increased levels of psychological distress among the survey respondents.
They found that healthcare workers who cared for fewer COVID-19 patients faced higher levels of PTSD, which may be due to the fact that these workers had less experience and therefore felt less prepared. The same was true of healthcare workers who cared for fewer patients during the SARS outbreak.
The authors also found that non-clinical healthcare workers — for example, administrative assistants or environmental staff — reported the highest levels of depression and anxiety. These employees may have received less pandemic-specific training and education than their clinical colleagues, leading to higher levels of psychological distress.
“It is imperative for healthcare institutions to not overlook the need for strong communication, educational interventions, and psychological support for all categories of [healthcare workers], both clinical and non-clinical,” the authors said.
Going forward, the team hopes that their results can be used to promote mental health and wellness among all healthcare workers.
While previous experience with an infectious disease outbreak doesn’t increase employees’ chances of facing psychological distress, other factors do — and creating mental health resources specific to these factors will help everyone get through the COVID-19 pandemic.