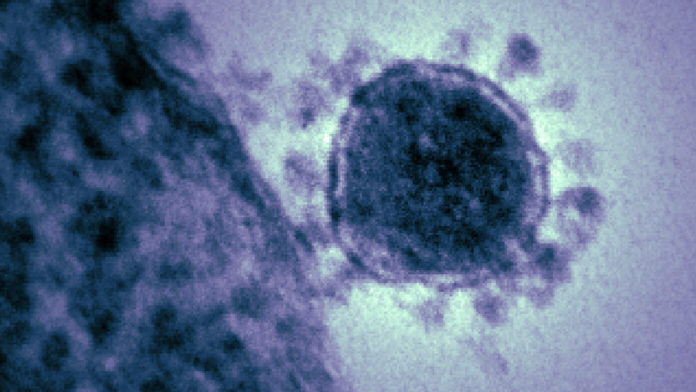
With the news that hundreds of people have been infected and dozens killed, the novel coronavirus pandemic has put the public on high alert. In Canada, there is increased airport screening for travellers with flu-like symptoms, and face masks are flying off the shelves.
But based on what we know so far, are these measures warranted and effective, or are there better ways to protect ourselves from deadly infectious diseases?
Quarantine unlikely to work, and infringes on civil liberties
The coronavirus family can sometimes be the pathogen that causes the common cold, but more serious outbreaks of strains like SARS (2003) and MERS (2012) have killed hundreds. It may seem only prudent to be as cautious as possible in trying to contain another potential major outbreak, but there are drawbacks.
At the moment, it’s a waiting game as we learn more about the new virus and how it’s transmitted, but the outbreak is already causing infringements on civil liberties. China has put the entire city of Wuhan, and the nearby cities of Huanggang and Ezhou, under quarantine. That’s an unprecedented attempt to contain 18 million people by shutting down transport by air, train, ferry and subway.
It’s a precaution that shocked Steven Hoffman, professor of global health, law and political science at York University. It’s also the kind of broad restriction that would likely also be illegal in Canada because of the protections offered by the Canadian Charter of Rights and Freedoms, Hoffman told Global News. The federal Quarantine Act would only extend to the isolation of specific individuals who would be a risk to public health.
But beyond that, it’s simply unlikely to work. The new coronavirus has been circulating since late December 2019, and people carrying it start shedding it long before symptoms emerge. Even airport screening is likely to fail because it relies on self-reporting, and tired travellers may hide their symptoms if they fear a quarantine might prevent them from going home.
Risk seems lower than for previous outbreaks, like SARS
The good news is that the novel coronavirus seems to be less transmissible and less severe than SARS.
“It’s both of those things that will tell us whether it will be a problem around the world,” said Allison McGeer, professor of epidemiology at the University of Toronto’s Dalla Lana School of Public Health, in a press release.
“If there’s sustainable human-to-human transmission, but the real case fatality rate is 1 in 80,000 – well, that’s another cold. It’s not nothing but it’s not a big deal. If there’s not sustainable person-to-person transmission, it doesn’t matter how severe it is — we can deal with it.”
So far, it looks like most cases are coming directly from contact at the seafood market where the virus originated, and beyond that human-to-human transmission is more or less limited to close contact, like spreading through a household. Compared to SARS, far fewer healthcare workers are being infected.
“During the SARS outbreak, about 20 percent of the cases worldwide occurred in healthcare workers,” added McGeer. “That’s good news on two fronts. First of all, it tells you that it’s not as transmissible person-to-person since health-care workers are up close and personal with severely ill patients and, secondly, it means it’s much less disruptive to the health-care system because we don’t have to be as worried.”
From the first case of the novel coronavirus on Dec. 12 to its identification as an outbreak on Dec. 29, there were 30 reported cases. Not a single healthcare worker was among them, despite not having any additional precautions in place. By contrast, a single case of SARS in Toronto spread to 50 healthcare workers in a week.
Proper hygiene and a flu shot go further than a face mask
For now, public health officials are simply advising Canadians to do what they should already be doing during any normal winter season: cough or sneeze into a tissue and throw it away immediately, wash your hands and disinfect common surfaces frequently, avoid close contact with sick people and stay home if you’re sick, and get the flu shot. The flu causes about 3,500 deaths in Canada every year, and because there is no vaccine for the coronavirus, that makes the flu a much more important target for any preventative measures that people can take.
Masks, even the coveted N95, are not recommended for preventative use by healthy people. It has no proven benefit and it can drain resources where they are actually needed, like putting a mask on a person with relevant symptoms who needs to enter a healthcare facility.
For now, there are a lot more reasons to be hopeful than to panic, but anyone who is concerned they may be experiencing symptoms of the coronavirus should still contact their primary care provider, local public health office, or call 811.