What does detecting bacteria in chronic wounds have in common with accurate removal of breast tumours? At first glance, not much. Looking closer, both of these medical conditions require doctors to see the invisible: to find microscopic bacteria in wounds, and to define the edges of tumours that blend in with surrounding healthy tissue. Missing even a few bacteria or tumour cells can translate into dangerous infections or cancer relapse, respectively.
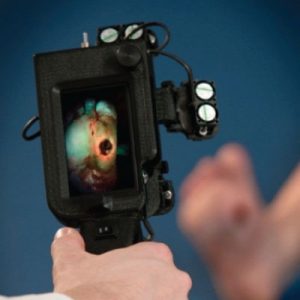
To overcome these challenges, Canadian molecular imaging scientist Prof. Ralph DaCosta and colleagues at the Princess Margaret Cancer Center and Techna Institute (University Health Network, Toronto), developed a handheld imaging device named PRODIGI.
PRODIGI stands for Portable Real-time Optical Detection Identification and Guide for Intervention, a name that captures the function of the device in clinical application. It enables surgeons and doctors to visualize and treat infection-causing bacteria or cancer-causing tumour cells in real-time.
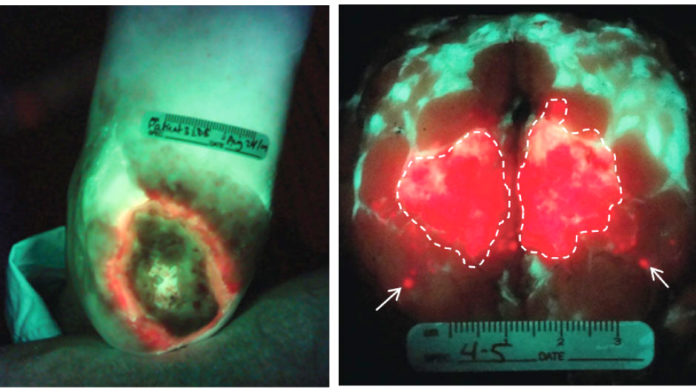
To do this, PRODIGI detects fluorescent light. Some bacteria naturally emit red fluorescence, so they can be seen without any special treatment. Some anti-cancer drugs can also cause selective tumour fluorescence, which causes tumours to fluoresce red, allowing PRODIGI to locate cancers based on where the drugs accumulate during treatment.
The concept for a handheld imaging device was born out of Prof. DaCosta’s PhD thesis where he helped develop systems for early detection of gastrointestinal cancers. By adapting these large, complex, expensive technologies into a portable device, Prof. DaCosta realized that this powerful imaging technology could have additional applications, including for the diagnosis of chronic wound infections.
Already in clinical trials, PRODIGI has been shown to detect and track bacterial infection in wounds in real-time, enabling early identification of infection, as well as more precise wound swabbing, treatment guidance, and tracking of treatment response. Based on these features, PRODIGI increases the rate of wound closure compared to the current standard of clinical wound examination. This is particularly significant in cases where urgent clinical attention is needed in patients who do not show the typical symptoms of wound infection.
PRODIGI is also being tested clinically at the Princess Margaret Cancer Center as a surgical guidance tool to improve the accuracy of breast tumour removal. Using drug therapy that creates a specific red fluorescent signal in tumours, PRODIGI can be used to detect the presence of residual tumour cells during surgery, therefore guiding more accurate removal of the entire tumour.
PRODIGI is being developed as both a handheld device and smartphone-compatible imaging device by Moleculight Inc., a company founded by Prof. DaCosta in 2012. Additional applications for the device beyond chronic wounds and breast cancer are also being developed. Can you think of other ways that PRODIGI can be useful? Feel free to include your ideas in the comments below.