In 2015, the Truth and Reconciliation Commission of Canada’s Calls to Action documented the systematic suppression of traditional Indigenous health knowledge and healing practices. This colonialist legacy persists today in the inadequate and inequitable access to healthcare experienced by too many First Nations, Inuit, and Métis Peoples across the country.
Now, a recent study from the University of Manitoba has shown that Indigenous-led health service partnerships may be one way we can work towards addressing these healthcare inequities.
Indigenous-led healthcare partnerships are “autonomously grounded in traditional Indigenous knowledge—maintained and upheld by local Elders, healers, and Knowledge Keepers”, and have demonstrated improved health outcomes for Indigenous Peoples across Canada, according to the study.
The study was published in the Canadian Medical Association Journal, and includes a detailed set of recommendations for future Indigenous-led healthcare partnerships.
Indigenous Peoples face alarming health inequities
Indigenous Peoples across Canada face numerous barriers when it comes to accessing healthcare. This includes racism, aggression and disrespect, among many other systemic barriers and inequities.
What’s more, the typical biomedical approach to healthcare in Canada is not reflective of the cultural world views held by many Indigenous Peoples. Mental health services in particular are often unable to address cultural issues—for example, intergenerational trauma due to colonization—and the result is that many Indigenous patients are left without sustained access to the help they need.
Instead of relying on Western medicine, however, many communities are now turning towards Indigenous-led health partnerships. These partnerships are informed by traditional Indigenous knowledge, and maintained through the work of Elders, healers, and Knowledge Keepers in Indigenous communities.
There are a number of innovative Indigenous-led health partnerships within Canada, including Turtle Lodge in Manitoba. The founder of Turtle Lodge, Elder Dr David Courchene, is one of the authors of the study.
How do Indigenous-led partnerships improve outcomes?
The authors carried out a literature review of different models, geographies, and settings of Indigenous-led healthcare partnerships across Canada and listed the health outcomes that had been reported in each case. For example, some partnerships are located in urban geographies (i.e. cities), whereas others are located in remote geographies.
Throughout the literature, there were many examples of improved healthcare outcomes reported from Indigenous-led partnerships. For example, a clinic in Western Canada that had mental health patients interact with an Elder over the course of six months found that emergency department mental health visits decreased by 56% among participants up to a year after the study concluded.
While many other examples of positive outcomes exist and are documented in the study, the authors caution that there are issues with trying to quantify these outcomes using numerical evidence.
“[I]t is problematic, either quantitatively or qualitatively, to have to ‘prove’ traditional Indigenous knowledge in terms of the dominant Western research paradigm and culture,” the authors explain.
Assuming that Western medicine is the superior benchmark against which other methods must be compared is a problematic colonial approach, and may even limit our ability to appreciate the benefits of Indigenous practices on their own terms.
Recommendations for the future
While Indigenous-led healthcare partnerships are certainly beneficial for Indigenous Peoples, the authors note that healthcare practitioners of Western medicine need to be cautious and respectful when creating these partnerships. A better understanding of how to protect and properly integrate Indigenous practices with Western practices is crucial if we want Indigenous-led healthcare partnerships to be successful.
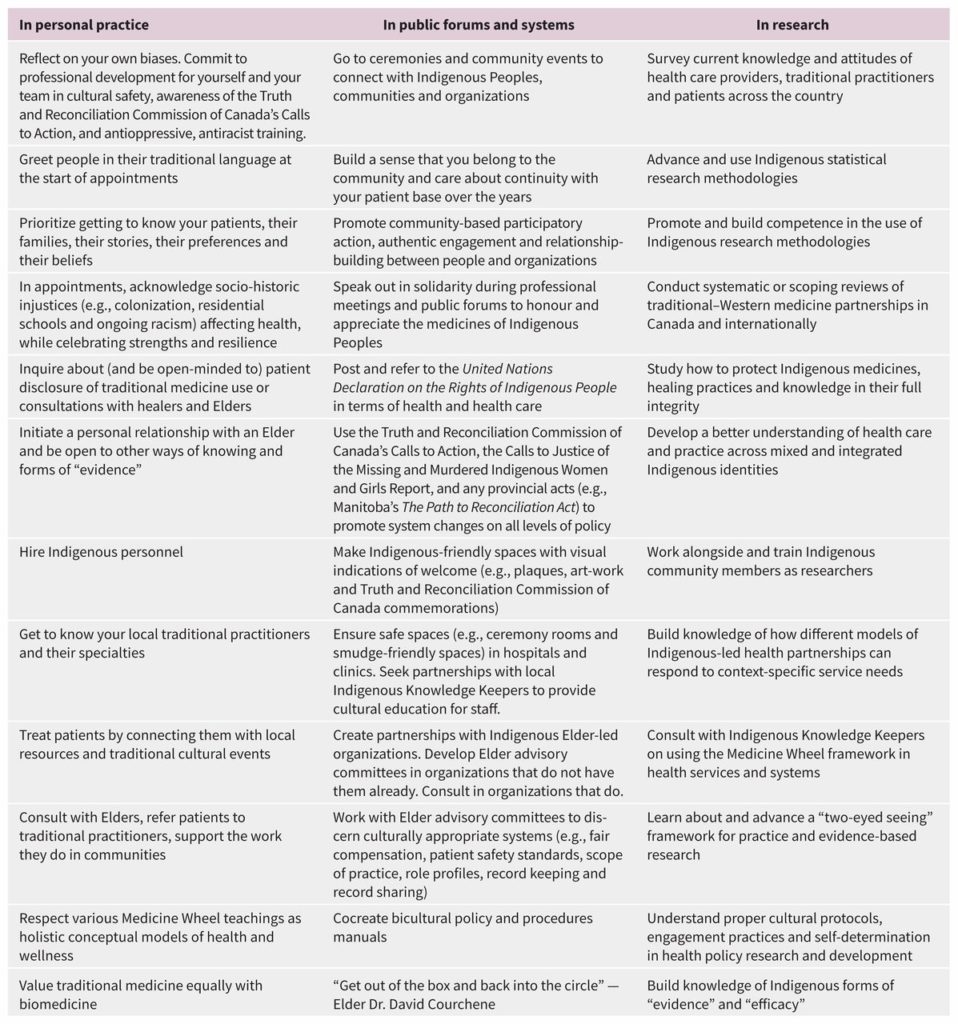
The Indigenous Physicians Association of Canada (IPAC) recommends that equal values are placed on Indigenous medicines and biomedicine when forging partnerships, and that healthcare practitioners are open to patients disclosing the use of traditional medicines. A number of additional recommendations are listed in the study.
The authors also include their own list of recommendations to complement those of the IPAC. These include hiring Indigenous personnel and getting to know local traditional practitioners, among others.
Overall, the authors see Indigenous-led partnerships as a promising opportunity that will flourish with the right support.
“[W]e view these Indigenous-led partnerships as opportunities for people from different cultures, health systems, and world views to benefit from learning about and accepting each other,” the authors conclude.
“If the swell of efforts of Elders, Knowledge Keepers, and healers can be supported by the larger medical community, and if barriers to full healthcare rights for Indigenous Peoples can be lessened or removed, then systemic racism can be overpowered and health equity can more easily be approached.”








































