It’s official: COVID-19 is a pandemic. This is a global health threat of the highest level.
It’s no longer a question of whether Canada will soon be dealing with a health emergency, but a question of when. But there may still be time to act so that our healthcare system doesn’t get completely overwhelmed with a surge of patients.
It’s a concept being described as flattening the curve: if it’s impossible to contain the spread of the virus that causes COVID-19, even spreading out the same number of infected Canadians over more time will help limit the number of patients that need to be treated at once. That alone will help keep the mortality rate down. And we need to start immediately, before the crisis escalates.
Because there is no vaccine or specific immunity against SARS-CoV-2, the coronavirus that causes COVID-19, the intervention is a social one. It relies on people voluntarily practicing social distancing by avoiding large crowds and working from home where possible, even before symptoms appear. People can be infected long before they know it. Unlike quarantines that limit individual civil rights, it’s a collective responsibility to do what’s right, even if it’s inconvenient.
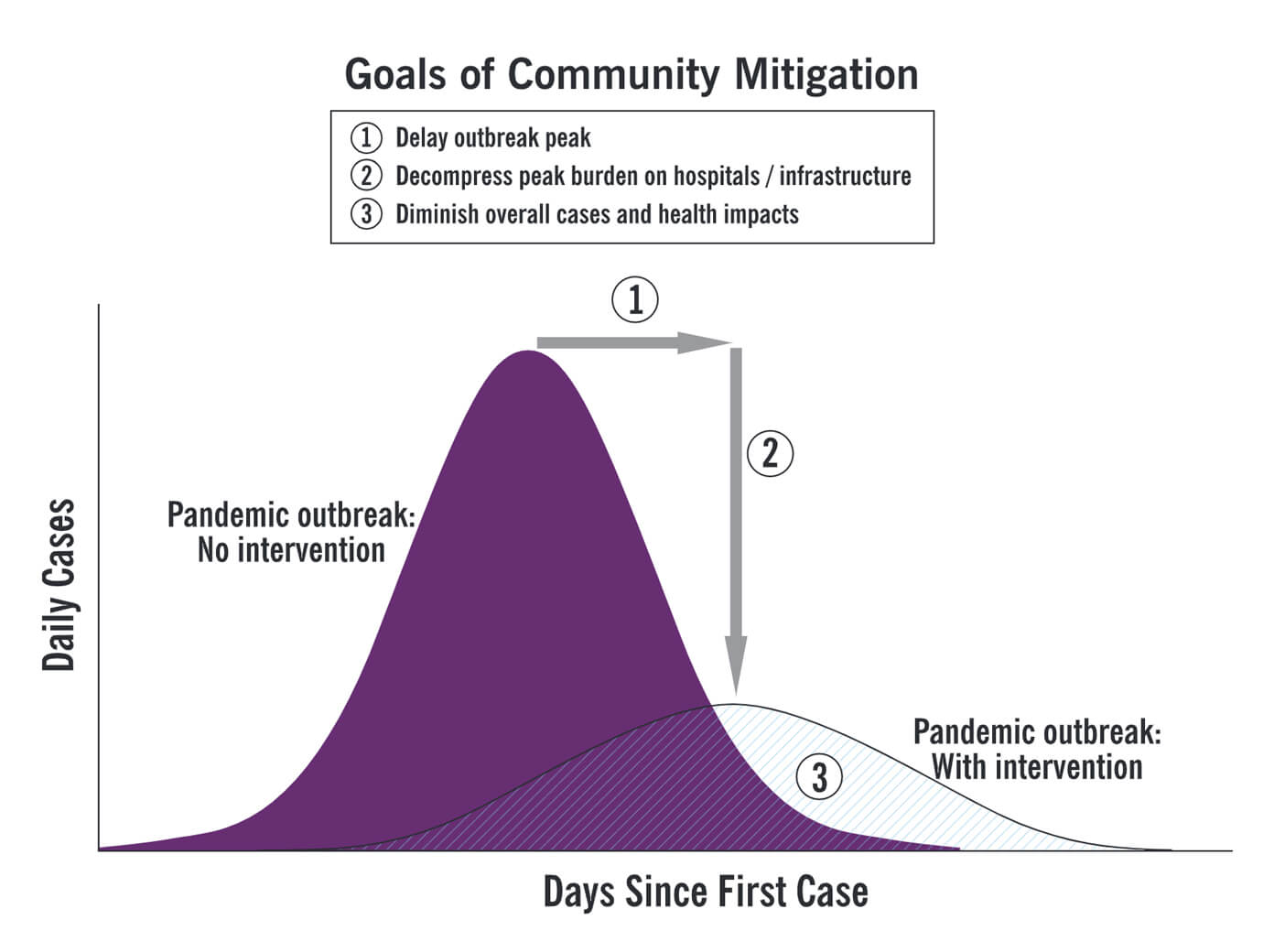
This is a great visualization of how social distancing works, and how it differs from inaction or from quarantine.
In tandem, our government also needs to step up with policies to support Canadians with access to social assistance for lost wages and childcare for people staffing essential services.
Limiting our face-to-face interactions will delay the peak of the outbreak, decrease the height of the burden on hospitals, and hopefully even diminish the overall number of cases.
Until now, Canada has had the luxury of giving the highest standard of care and caution because there has been a very low number of local COVID-19 cases. If the number of cases rises sharply, the strain on the healthcare system will mean a much higher mortality rate.
Hospitals are already stretched to the limit with space and resources for patients. A sudden influx of patients who require isolation, beds, and ventilators can easily inundate a system that doesn’t have the capacity to spare.
In Italy, a country with a strong healthcare system, the death toll is rising exponentially as doctors are struggling to make heartbreaking choices on which patients to treat, given their limited resources. On the high end of current projections that 60 percent of adults may get infected, a surge of cases also means a surge of sick healthcare workers.
And it’s not just about the virus’s direct effect, but about how our entire system is set up. Even unrelated medical conditions will be hit hard by a steep peak of COVID-19 cases as beds and doctors get pulled away. We also rely heavily on offshore drug supply chains, as many drugs used here are made in China and India, and we are already seeing disruptions.
This is the world’s first pandemic caused by a coronavirus, and contrary to what many people might initially think, it’s the low case mortality rate that makes this outbreak so effective. At around 2 or 3 percent, it’s much lower than SARS (10 percent) or MERS (34 percent), and yet COVID-19 has already claimed more lives than both combined.
Many infected people will only ever have mild symptoms, and others can be contagious before their conditions worsen, but as they continue with their daily lives they can spread it to others who may not be so lucky. People should also be aware that the number of confirmed cases will always lag behind the true number of people who are carrying the virus and aren’t yet experiencing symptoms, or that their symptoms haven’t become severe enough to seek treatment or a diagnosis. Those silent numbers are worrying.
In the best case scenario, Canadians will be able to walk away from this outbreak feeling like all these precautions were an overreaction, while in truth we dodged a disaster. The flip side is that we wait too long for action and the worst case hits, and the damage grows exponentially. Hopefully our collective action will have a positive impact.